When you’re experiencing excruciating back pain, it overtakes your entire life. Every waking moment you’re reminded by the pulsating pain that just doesn’t seem to go away. As a last resort, you turn to epidural steroid injections – but the pain gets worse.
But wait, aren’t steroid injections that your doctor enthusiastically recommended supposed to make the pain go away? Not necessarily.
Unfortunately, many people who experience intense back and neck pain are left with little to no other options. That is, if they turn to their medical doctors for help managing the pain. When it comes to back pain, medical doctors often recommend pain-killers like ibuprofen, or prescription-only NSAIDs like diclofenac (Voltaren), or celecoxib (Celebrex). If those don’t work, they’ll often recommend epidural steroid injections, which come with some terrifying risks.
What Are Epidural Steroid Injections
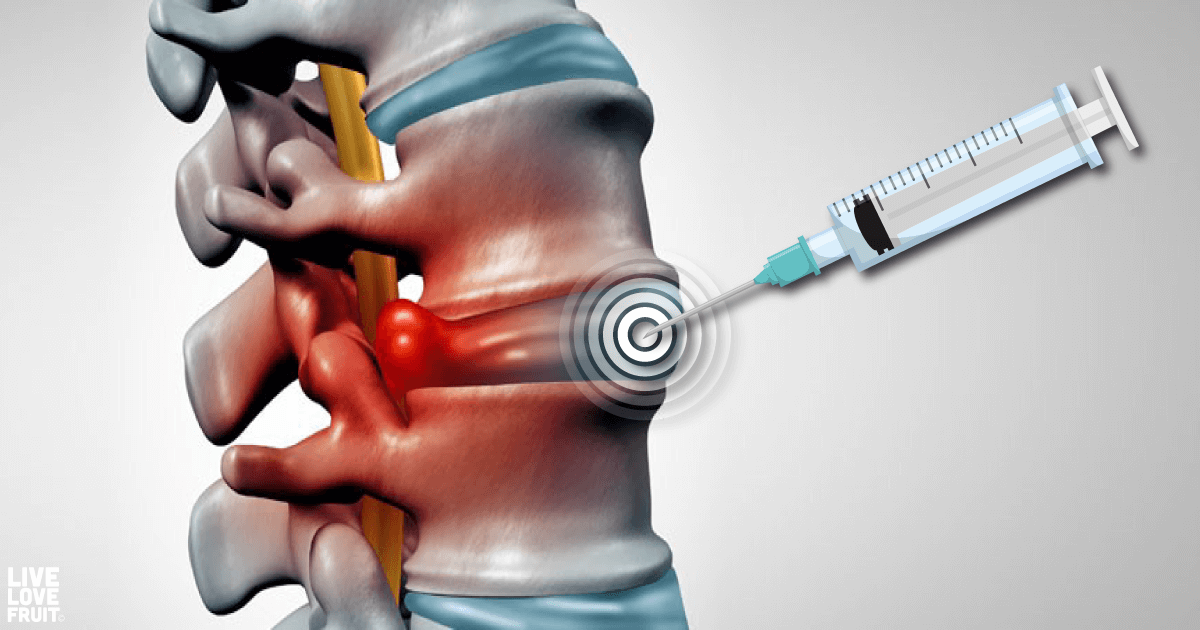
Epidural steroid injections are a treatment option commonly used for low back and leg pain. They have been used for low back problems since the early 1950’s, and are currently used for non-surgical management of sciatica and low back pain (1).
To help a patient relieve spinal pain, a doctor will inject the epidural space (between the spinal cord and bony structure of the spine) with steroids.
The injection usually consists of (2):
– Steroids or cortisone (anti-inflammatory agent)
– Lidocaine (fast-acting local anesthetic)
– Saline (dilutes local anesthetic)
Once the steroids are injected, the mixture is supposed to have an anti-inflammatory effect that can last anywhere from a few days to a few months (3).
Unfortunately, the epidural space is a very delicate part of the body, making the procedure extremely risky.
The Risks of Epidural Steroid Injections
In April 2014, the U.S. Food and Drug Administration (FDA) issued a drug safety communication entitled “FDA requires label changes to warn of rare but serious neurologic problems after epidural corticosteroid injections (ESI) for pain (4).” The FDA’s warning even stated that they could “result in rare but serious adverse events, including loss of vision, stroke, paralysis, and death (5).”
The side effects of epidural steroid injections are so severe that the FDA ruled that all injectable steroid must carry an updated warning that includes the above risks, as well as “arachnoiditis, bowel/bladder dysfunction, headache, meningitis, paraparesis/paraplegia, seizure, [and] sensory disturbances (6).”
The FDA’s website also warns that “the effectiveness and safety of injection of corticosteroids into the epidural space of the spine have not been established, and FDA has not approved corticosteroids for this use (7).” This is largely due to the fact that research into the risks of epidural steroid injections is still being conducted. Approved or not, Dennis Capolongo of the ENDC, a ground that has campaigned against epidural steroid injections for years, believes that warning labels need to be stronger, and more visible – not just confined to the small print.
Australia and New Zealand updated their warnings in February 2018, such that steroid injections “MUST NOT be used by the intrathecal, epidural, intravenous or any other unspecified routes (8).” Unfortunately, this isn’t the case for corticosteroid injections in the USA, as doctors still use them for purposes that carry much too heavy of a risk.
In a forum on SPINE-health, one woman with pain in her lumbar spine described her first steroid injection as following:
“I don’t know what went wrong, as was told I’d feel a couple of bee stings, then maybe some pressure. I have a new scale for pain now, and on a scale of 1-10, it was 15. The most excruciating pain I’ve ever experienced. I passed out from it, and my blood pressure dropped to 78/52. They had to give me oxygen, smelling salts, wet towels, etc. They will NEVER do that to me again. Intensely painful and a nightmare.”
Another woman, Helen Bertelli, was diagnosed with arachnoiditis, an incurable condition that can be associated with epidural steroid injections. After her epidural steroid injections for back pain, she started feeling electric shocks, muscle cramps, and a sensation of water running down her legs (9). “I had this feeling I was connected to the end of a guitar string and someone was plucking it. My legs just exploded like there were fireworks in them. My muscles twitched like they were boiling.”
While this pain-relieving procedure may initially provide some relief, the scary symptoms and risks make it not so worth it.
What You Can Do Instead
While seeking medical aid from a doctor is important if your back pain came on suddenly, or if your back pain is so bad that day-to-day life becomes a constant struggle, managing back pain can be much simpler than you think. While it may require a little effort on your behalf, managing back pain doesn’t always have to be remedied with epidural steroid injections.
If you haven’t tried the following suggestions to help remediate your lower back or hip pain, I recommend giving them a try!
Stretch
This one might seem obvious, but I’m serious when I say stretch! Regular stretching helps protect your back by increasing flexibility and decreasing the risk of injury. A lot of people go for epidural injections for sciatica pain to release the sciatic nerve. However, more often than not, the sciatic nerve is being pinched by a tight piriformis muscle, which needs to be released. Check out my article on stretching the piriformis, and if your issue is more back-related, I have tons of articles on stretching out the muscles that trigger tightness in the back muscles.
Eat an Anti-Inflammatory Diet
Consuming an anti-inflammatory diet is crucial if you’re wanting to live pain-free. Many foods have been shown to reduce (or increase) inflammation, a known cause for back pain and inflamed nerves (which epidurals are designed to alleviate). So when you have back pain, changing your diet may help you avoid it.
Eating a mostly plant-based diet, which includes anti-inflammatory foods like chia seeds, broccoli, leafy greens, turmeric, watermelon, and the like, is a great option to help reduce body aches and pains. It is also important to reduce the consumption of foods that cause chronic inflammation in the body like wheat, refined sugar, trans fats, conventional meats, dairy and vegetable and seed oils.
Also, don’t forget to drink enough water! Drinking 3-4 liters a day will ensure you’re flushing out all the acidic waste deposits that contribute to body pain.
Essential Oils
Utilizing pain-relieving essential oils in your day-to-day regimen to alleviate different aches and pains is actually more effective than you might think. Studies have found that applying essential oils on the skin allow their natural components to absorb into the bloodstream (10). So while you may think that putting essential oils on the skin and area of pain is pointless, it actually really works (I can attest to this myself!).
One of my favorite pain-relieving essential oils is copaiba essential oil, which contains the cannabinoid beat-caryphyllene (BCP). It specifically targets CB2 receptors, which aid in the reduction of inflammation and pain.
Other pain-relieving essential oils include things like rosemary, frankincense, myrrh and spruce.
Prolotherapy
Prolotherapy is a natural, alternative therapy, also known as regenerative joint injection or non-surgical ligament and tendon reconstruction. Prolotherapy is a procedure whereby a natural irritant is injected into the soft tissue of an injured joint or spine, which then kick-starts the body’s healing response. Prolotherapy can be expensive, but the results, according to many, are very worth it.





Very conflicting messages from different people.
I am schedule in 3 weeks for an epidural steroid but now I am reluctant and may postpone or never do it. I have herniated disk betweenL4 and L5. for over 6 weeks now… They call it sciatica.
Pain is being managed by opiods for short term celebrex works well non-addictive for long-term.
But what has helped me short immediate term is a Toradol shot intramuscular on buttocks and is a strong anti-inflammatory as well. Have you tried this.
Hopefully we could advance to laser surgeries sometime in the future.
Hoping for the best for you.
I have never had any shots or steroid shots, I only wrote the article with studies I researched. I hope you can make the right decision for yourself!
Did you get the injections? See my post below about my son , similar to yours .
I have had many injections. Last one 2 years ago. When I worked I got them every 8 months. I totally trust my doctor. I never had an issue. And the really help me.
So glad they helped you Marie, others have not been as fortunate as you. Please listen to Gary’s recent testimony to the FDA/AADPAC Advisory Board and you’ll see what I mean. https://youtu.be/-w-nzvg3br8 The fact that you need repeated injections only means the underlying issues have not been properly addressed… but I fully understand. So please be careful, one slip and your life could be forever changed.
I had the injections no problem and I felt a little pressure no pain at all. If the doctor doesn’t give the numbing agent a chance then you might feel pain. My doctor is great he knows what he is doing.
Same here i have no choice. thinking about trying the CBD cream rub for the pain down the back of my legs to my toes. i just had the injections last year. some of the meds i was taking had me stoned out of my head. i am currently on 2 meds that do not upset my stomach. alogn with tylenol extra strength
Chiropractors do this the best!!!!
Good Day i do have the injections in my back last 4 injesctions along with stretches excercise i have the pain radiating down my back to my toes excru ciating.. since 1999, I have tried all kinds of meds some sent me into another world. currently i have 2 meds Soma, Gabapentin, i take Tylentol in the mid of the day. i tried everything to a point i developed stomach problems. i have no idea what else to do to help the back pain. the pain gets so bad i cannot sit on the toilet and try to stand all day afraid ,along with the cramping in the legs.,Pt, Chiro. thinking of using the new cbd oil for the arthuritis its the cream rub some people are using and state its helping. I wish you the best
Dear Rose, there is no “conflicting” messages… just those that know the truth and the facts, and those that do not. Remember, there are no magic bullets, no pill, no injections that will heal your body… only time and gentle loving care. For centuries people have cured themselves by being patient and NOT in a rush. Lay off your back, no chiropractic, gentle massages, simple exercises, etc. If your injury is severe, ESI’s will not do anything, even possibly make things worse… only corrective surgery will. But if its simple sciatic pain, the body will heal the disc, if giving the time and proper care. Pfizer recently asked the FDA to ban their steroids for ESI’s. In fact there are no injectable steroids made by anyone that are approved for ESI’s anywhere on Earth due to reports of severe adverse events including death. Ask this question to your doctor as a litmus test. “Hey doctor, are these injection approved by the FDA?” If he/she says “YES” then run… if he/she says “NO” then ask “Why not?” They make $2500.00 an injection… very lucrative, that’s their motivation. In fact according to the 2014 FDA AADPAC hearings on the safety and efficacy of ESI’s, they determined that less than <28% report some type of SHORT-TERM benefit (none long term) while the remaining 72% reported either no change in symptoms, an increase of pain symptoms, new unexplained symptoms, or suffer from a catastrophic medical event. The FDA also reported that X-Ray guided fluoroscopy does not reduce these risks. Pfizer also claims that "ESI's are not a cure" on their most recent Data-sheet. Please take care!
Thank you Dennis! I was scheduled this morning for an Epidural and cancelled due to your valuable information.
You’re indeed very welcome! Don’t forget to thank Carly as well for setting up this blog. If you ever wish to contact the EDNC, our email address is [email protected] : )
Hi, hope you can help. In your research did you find anything for cervical cancer/pinched nerve w/arthritis? I have metasized cancer to my neck and spine. That said, I do have a all my pain in my neck, shoulder blade and numbing in hand in forearm. I am on cbd pain cream which helps me to sleep, tried PT to my disheartening it failed to relieve pain. So what to do? Surgery, NO since I will have to stop all my cancer treatment, so I am thinking of the steriod injection. Ugh..what to do?
your comments appreciated
Irene
Hey Irene, I think this is a really long, complicated answer that doesn’t just end with “get the steroid injections to help your pain” – I would suggest working with an integrative medical doctor to look at everything in a more wholistic way (or even a naturopathic doctor at that).
Hi Irene, I too suffer from a similar diagnosis. So may I add my two cents? Back in 2014 the United States Food & Drug Administration held an advisory committee hearing (AADPAC) on the safety and efficacy of Epidural Steroid Injection therapy for acute pain conditions of the spine. (Not chronic nor systemic) After three days of presentations, public testimony and private meetings, the FDA held a vote on whether there was enough evidence to now issue a “Contraindication for epidural administration” of injectable steroids, specifically in the Cervical spine.
The vote was 15-YES, 7-NO with 1-Abstention. The advisory panel had spoken, they wanted it banned at least for the cervical spine.
However, based on documents obtained by the EDNC, the FDA intentionally withheld vital information from those at the hearing. One year earlier in 2013 the makers of the most commonly used off-label steroid, Pfizer’s Depo-Medrol, issued new global label-change Warnings to the CORE data-sheet. They decided that because of increased adverse medical event reports including arachnoiditis, permanent paralysis and death they now wished to have their drug “Contraindicated for Epidural Administration” at ALL LEVELS of the spine, adding a ”MUST NOT USE via the epidural route” Black-Box WARNING to the label. Many nations including New Zealand, Australia, South Africa, Brazil, Canada, Italy, France, Switzerland, Russia etc have all agreed to Pfizer’s Global CORE Warning changes without hesitation.
Most importantly, Pfizer clearly states that their product (Depo-Medrol® or Methylprednisolone Acetate) should not be used via the epidural route, nor should it be be considered a cure. In fact it also says that it should not be administered into cancers. These warnings typically apply across ALL injectable steroids since NONE are approved for epidural administration by any health authority anywhere on planet Earth.
Despite all the presented evidence to the FDA, along with a majority vote by their own Safe Use Initiative and AADPAC Advisory teams, plus a manufacturers’ demand for an Epidural Contraindication CORE change, the US-FDA once again caved to the lobbying pressures of the $300B Epidural Steroid Injection industry and said “NO” to all these groups along with the manufacturer! (Documents to substantiate these claims are available here: https://jmp.sh/5rBMDyq and here: https://jmp.sh/uxCiBGK)
Wow. My 36 year old son just had ESI in back last week . He’s getting the fireworks like pain described above with little relief . Almost had to take to ER 36 hours after injections. Everyone says keep trying this before surgery . So scary . He has 2 herniated discs , or protrusions/ extrusions as they call them in the MRI . Then others said , he’ll have to have surgery ?? Go see a surgeon ASAP . Help
Gail, please contact The EDNC if you seek answers. We are a nationally recognized Patient Advocacy Collaborative specializing in adverse ESI outcomes. You can find us on the net or e-mail the campaign directly at [email protected]
What about just lidocaine in the muscle? Is that dangerous as well?
I would personally stay away from all injections if it were my body, but that’s just me. Always do your research and choose what you think would serve your body best.
I have had sciatic pain for years, resulting in fusion with metallic support in 1994. It was a slight relief after the surgery, which took several months to “recover”.I learned to live with pain, which sucks the energy from my life. I had a bi-lateral epidural about 6 months ago.My fusion was the classic L4-L5 with hardware. My present orthopedist wants to fuse L2 to S1. Since the epidural I have no shooting pain, but still extreme lower back muscular pain when standing or walking. with the added side effect of having both right and left lower legs going gradually from tingling tocomplete numbness in both feet. It’s hard to walk without a cane when feet are numb. My sensors which used to give feedback are not functioning. There is still severe lower back pain. Now what? I would trade my previous sciatica in one leg for my present condition.
Think long and consider possible side effects of epidural injections before going that route.
Sorry you’ve had to go through that. I would recommend seeing a physiotherapist or manual osteopathic practitioner.