When you’re experiencing excruciating back pain, it overtakes your entire life. Every waking moment you’re reminded by the pulsating pain that just doesn’t seem to go away. As a last resort, you turn to epidural steroid injections – but the pain gets worse.
But wait, aren’t steroid injections that your doctor enthusiastically recommended supposed to make the pain go away? Not necessarily.
Unfortunately, many people who experience intense back and neck pain are left with little to no other options. That is, if they turn to their medical doctors for help managing the pain. When it comes to back pain, medical doctors often recommend pain-killers like ibuprofen, or prescription-only NSAIDs like diclofenac (Voltaren), or celecoxib (Celebrex). If those don’t work, they’ll often recommend epidural steroid injections, which come with some terrifying risks.
What Are Epidural Steroid Injections
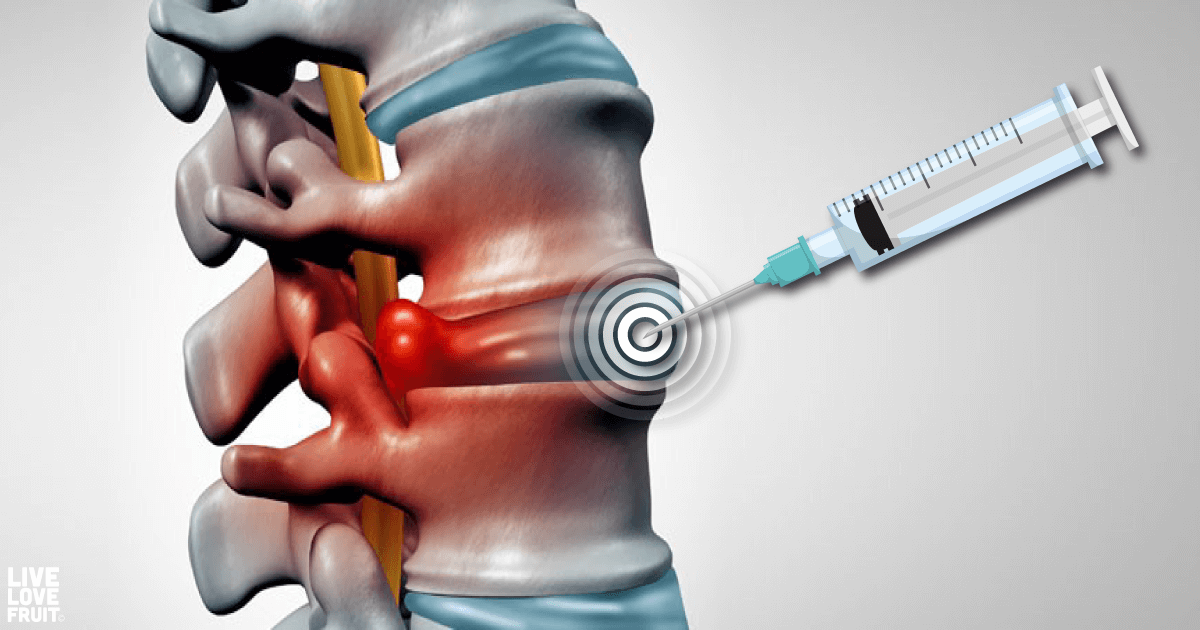
Epidural steroid injections are a treatment option commonly used for low back and leg pain. They have been used for low back problems since the early 1950’s, and are currently used for non-surgical management of sciatica and low back pain (1).
To help a patient relieve spinal pain, a doctor will inject the epidural space (between the spinal cord and bony structure of the spine) with steroids.
The injection usually consists of (2):
– Steroids or cortisone (anti-inflammatory agent)
– Lidocaine (fast-acting local anesthetic)
– Saline (dilutes local anesthetic)
Once the steroids are injected, the mixture is supposed to have an anti-inflammatory effect that can last anywhere from a few days to a few months (3).
Unfortunately, the epidural space is a very delicate part of the body, making the procedure extremely risky.
The Risks of Epidural Steroid Injections
In April 2014, the U.S. Food and Drug Administration (FDA) issued a drug safety communication entitled “FDA requires label changes to warn of rare but serious neurologic problems after epidural corticosteroid injections (ESI) for pain (4).” The FDA’s warning even stated that they could “result in rare but serious adverse events, including loss of vision, stroke, paralysis, and death (5).”
The side effects of epidural steroid injections are so severe that the FDA ruled that all injectable steroid must carry an updated warning that includes the above risks, as well as “arachnoiditis, bowel/bladder dysfunction, headache, meningitis, paraparesis/paraplegia, seizure, [and] sensory disturbances (6).”
The FDA’s website also warns that “the effectiveness and safety of injection of corticosteroids into the epidural space of the spine have not been established, and FDA has not approved corticosteroids for this use (7).” This is largely due to the fact that research into the risks of epidural steroid injections is still being conducted. Approved or not, Dennis Capolongo of the ENDC, a ground that has campaigned against epidural steroid injections for years, believes that warning labels need to be stronger, and more visible – not just confined to the small print.
Australia and New Zealand updated their warnings in February 2018, such that steroid injections “MUST NOT be used by the intrathecal, epidural, intravenous or any other unspecified routes (8).” Unfortunately, this isn’t the case for corticosteroid injections in the USA, as doctors still use them for purposes that carry much too heavy of a risk.
In a forum on SPINE-health, one woman with pain in her lumbar spine described her first steroid injection as following:
“I don’t know what went wrong, as was told I’d feel a couple of bee stings, then maybe some pressure. I have a new scale for pain now, and on a scale of 1-10, it was 15. The most excruciating pain I’ve ever experienced. I passed out from it, and my blood pressure dropped to 78/52. They had to give me oxygen, smelling salts, wet towels, etc. They will NEVER do that to me again. Intensely painful and a nightmare.”
Another woman, Helen Bertelli, was diagnosed with arachnoiditis, an incurable condition that can be associated with epidural steroid injections. After her epidural steroid injections for back pain, she started feeling electric shocks, muscle cramps, and a sensation of water running down her legs (9). “I had this feeling I was connected to the end of a guitar string and someone was plucking it. My legs just exploded like there were fireworks in them. My muscles twitched like they were boiling.”
While this pain-relieving procedure may initially provide some relief, the scary symptoms and risks make it not so worth it.
What You Can Do Instead
While seeking medical aid from a doctor is important if your back pain came on suddenly, or if your back pain is so bad that day-to-day life becomes a constant struggle, managing back pain can be much simpler than you think. While it may require a little effort on your behalf, managing back pain doesn’t always have to be remedied with epidural steroid injections.
If you haven’t tried the following suggestions to help remediate your lower back or hip pain, I recommend giving them a try!
Stretch
This one might seem obvious, but I’m serious when I say stretch! Regular stretching helps protect your back by increasing flexibility and decreasing the risk of injury. A lot of people go for epidural injections for sciatica pain to release the sciatic nerve. However, more often than not, the sciatic nerve is being pinched by a tight piriformis muscle, which needs to be released. Check out my article on stretching the piriformis, and if your issue is more back-related, I have tons of articles on stretching out the muscles that trigger tightness in the back muscles.
Eat an Anti-Inflammatory Diet
Consuming an anti-inflammatory diet is crucial if you’re wanting to live pain-free. Many foods have been shown to reduce (or increase) inflammation, a known cause for back pain and inflamed nerves (which epidurals are designed to alleviate). So when you have back pain, changing your diet may help you avoid it.
Eating a mostly plant-based diet, which includes anti-inflammatory foods like chia seeds, broccoli, leafy greens, turmeric, watermelon, and the like, is a great option to help reduce body aches and pains. It is also important to reduce the consumption of foods that cause chronic inflammation in the body like wheat, refined sugar, trans fats, conventional meats, dairy and vegetable and seed oils.
Also, don’t forget to drink enough water! Drinking 3-4 liters a day will ensure you’re flushing out all the acidic waste deposits that contribute to body pain.
Essential Oils
Utilizing pain-relieving essential oils in your day-to-day regimen to alleviate different aches and pains is actually more effective than you might think. Studies have found that applying essential oils on the skin allow their natural components to absorb into the bloodstream (10). So while you may think that putting essential oils on the skin and area of pain is pointless, it actually really works (I can attest to this myself!).
One of my favorite pain-relieving essential oils is copaiba essential oil, which contains the cannabinoid beat-caryphyllene (BCP). It specifically targets CB2 receptors, which aid in the reduction of inflammation and pain.
Other pain-relieving essential oils include things like rosemary, frankincense, myrrh and spruce.
Prolotherapy
Prolotherapy is a natural, alternative therapy, also known as regenerative joint injection or non-surgical ligament and tendon reconstruction. Prolotherapy is a procedure whereby a natural irritant is injected into the soft tissue of an injured joint or spine, which then kick-starts the body’s healing response. Prolotherapy can be expensive, but the results, according to many, are very worth it.





I have currently had the spinal injections. It was the most excruciating pain I have ever had. The procedure was done 4 days ago and I am still in pain . I have had convulsions at the site and have continued to have pain. I have been sick, having severe hot flashes, have almost fainted and I have been sleeping almost on demand. I had a stroke in 2015 and told my doctor I think that surgery was a better option as I have extreme disc damage in my lower back. I am so not impressed that my doctor was not honest
Sorry to hear that Sharon – I hope you recover quick 🙁
I’ve had many injections and most lasted only three months. Some hurt afterwards and some not. The pain relief was well worth it. I had nerve damage between the L5-S1 and needed a spinal fusion. The last one I had was over a year ago. The pain left after 15 days. You need to take it easy afterwards and let the medicine work.
Also, don’t be afraid to switch doctors.
Also, usually they would only do two areas sometimes four. The last time the did eight. This worked. I still have pain at the end of the day if I over extend. But I now sleep through the night and wake refreshed. I have had some hot flashes and nausea but not every time. For some reason no two are the same. If the pain comes back I’ll be there again and pray the doctor has a steady hand and don’t move no matter what you feel, it’s not comfortable but it’s worth it.
Carly, I returned from Afghanistan last September I’m 52 years old this is my third trip down range and I’m hoping to get well for another one.
You may or may not know our body armor with ammunition emergency first aid signaling grenades and water is around 80 lb.
At a 7lb weapon or three thousand helmet 6270 lb pack and I suppose it’s no wonder that I finally succumbed.
My MRI shows sacroiliitis bursitis on my left greater trochanter and my symptoms indicate sciatica.
I’ve had some success with the epidural injections an SI injection Physical Therapy but I’m still not back to work after 3 months. Right now I’m good for about 2 hours a day and then I can’t stand to be on my feet anymore.
I’m desperate and I’m lapping up anything I can get.
Thank you for your consideration.
Hey Mark! So is your main issue your back, or sciatica, or both? Have you tried any of the stretching exercises on my website that pertain to sciatica and back pain? I’d also suggest going to a sauna or steam room to get heat into the areas in question. I’m also going to be investing in a Biomat soon, as they are 700x stronger than infrared sauna’s and it’s just a mat you lay down on. Apparently works well for lots of people with back/body pain. They are pricey, but worth it (I have a couple friends who use them, and have told me its the best investment they’ve ever made).
I had severe sciatic in 1999 caused by a ruptured disc. I had the epidural injections and it gave me immense relief after the 2nd injection. I had a series of 3 with no problems.
I’m glad the effects were not negative for you. I know a lot of people who’ve said these injections ruined their life. And the research to back it up is discerning. Maybe for some people the effect is the opposite? Flooks in the grand scheme of it all.
I have had spinal injections and I am at the point now I can barely stand up, walk or in so much pain. Loss of vision and i have bowel problems. I am miserable everyday of my life.
Sorry to hear that Victoria. Have you heard of the Biomat? They are expensive, but I’ve heard nothing but good things!!
I had prolotherapy in 2006 and it was incredibly effective. I had hip issues, had lower back pain since i was 28, and sciatica. It fixed all of it. Went back for a treatment in 2013 and am still doing fine. More people should try it.
Thanks for the note Megan! That’s great to know 🙂 I’ve heard really good things about it!!
About Prolotherapy, My wife had it! It’s a very cruel treatment and probably not FDA approved. Everyone needs to research it before trying it. I am surprised it was mentioned in the above story.
What happened to your wife? Something doesn’t have to be FDA approved to work. Lots of things aren’t FDA approved. The FDA also approves things that are later proven to be incredibly harmful. Kind of like epidural injections.