
Have you ever had a gut feeling or instinct about a certain situation or person? Turns out, you might be getting signals from an unexpected source: your second brain.
In recent years, there’s been a growing body of evidence that shows how our gut bacteria influences how we think and feel.
Our Gut and How We Feel
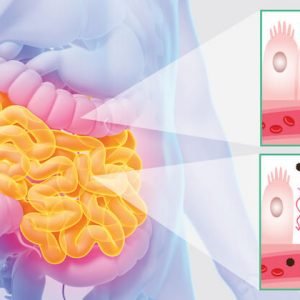
Scientists call this “brain in your gut,” the enteric nervous system (ENS). It is composed of two thin layers of more than 100 million nerve cells lining the gastrointestinal system all the way from the esophagus to the rectum (1).
These nerve cells control blood flow and secretions to help the gastrointestinal tract digest food and other particulate matter. They help us “feel” what is going on inside the gut, since they determine the mechanics behind food digestion.
While the ENS isn’t capable of political reasoning or in-depth thought, it does “communicate back and forth with our big brain – with profound results,” explains Jay Pasricha, M.D., director of the Johns Hopkins Centre for Neurogastroenterology (1).
For example, a troubled intestine can send signals to the brain, just as a troubled brain can send signals to the gut. Therefore, when someone is experiencing digestive distress, this can be the cause of emotional distress, or it can be the product of it.
When I was in university for five years of my life, I experienced heavy bouts of IBS that were directly related to the amount of stress I was putting myself through with heavy timetables and packed schedules. I am fortunate enough to say that since graduating, I rarely, if ever, experience bouts of IBS, and if I do, they are very minimal.
“For decades, researchers and doctors thought that anxiety and depression contributed to these problems. But our studies and others show that it may also be the other way around,” Pastiche says.
The ENS can be triggered by irritation to the gut (such as inflammation from sensitivities to certain foods), which can send signals to the central nervous system (CNS) that results in mood changes. This might explain why people with IBS and other bowel problems are more prone to develop depression and anxiety at some point in their life.
Our Moods Are Intimately Tied To Our Guts
When we’re stressed, our bodies react with a “fight or flight” response, which raises cortisol levels and thus, increases the stress response. While stress is a normal part of daily life, when it becomes chronic, our bodies remain in a constant state of inflammation (as a result of consistently higher cortisol levels) (2).
Research suggests that some people with functional GI disorders perceive pain worse than other people do because their brains can’t regulate pain signals from the GI tract. Stress can make the existing pain even worse (3).
Exposure to prolonged stress can result in high blood pressure to autoimmune disorders.
One study found that when a certain type of bacteria was given to mice that had similar behavioural characteristics as humans with autism, the gut microbiome of the mice changed, along with their behaviour. They became more social with other mice, and their anxious behaviour decreased significantly (4).
Another study investigating the effects of probiotic use and depression in patients with irritable bowel syndrome, found that those supplemented with probiotics saw dramatic improvements from depression. The patients took the probiotic Bifidobacterium longum NCC3001 every day (5).
These aren’t the only studies investing the effects of probiotics on mood, either. Several studies show evidence for reduced feelings of anxiety and improved aspects of well-being after taking probiotics (6, 7, 8).
Even gastroenterologists are starting to prescribe antidepressants to patients with IBS, because they seem to help calm symptoms by acting on nerve cells in the gut.
But we all know that if we simply feed our bodies properly, we don’t require medication.
Heal Your Gut, Heal Your Brain
With surmounting evidence on how supporting your gut microbiome can provide reduced psychological distress, it’s important to understand how to do just that.
There are a few things you should to to improve your gut-brain connection. Below are just a few key things you start doing today.
1. Eat Probiotics
Eating probiotic-rich foods like coconut water kefir, sauerkraut and kombucha, is a great way to get in your daily probiotics. They not only help improve mood, but are responsible for nutrient absorption, and strengthening your immune system.
I also suggest taking a daily probiotic if you can. My favourite are those by Puradyme. I’ve been using them for a solid year now, and have experienced a dramatic change in the way I feel, and also how I look. I used to suffer from a lot of bloating, no matter what I ate, but now I experience almost no bloating!
Probiotics by Garden of Life come in at a close second, and now I switch between Puradyme and Garden of Life every day to make sure my gut doesn’t get used to just a few strands of bacteria – but multiple strands.
2. Avoid Gluten and Processed Foods
I cannot stress how important it is to avoid gluten and processed foods. Ultra-processed foods like wheat bread, chips, and other treats dramatically alter the flora in our gut, which can directly translate to poor moods. Also, a lot of processed foods contain high-fructose corn syrup (HFCS), which increase the growth of bad bacteria like fungi and yeast.
3. Add Prebiotic Fibre To Your Diet
Prebiotics feed the growth of good bacteria, and since they aren’t as easily digested as probiotics, they actually make it all the way through the lower intestine. Foods that contain high levels of probiotics are chicory root, jerusalem artichokes, dandelion greens, garlic, asparagus and leek.
4. Exercise Regularly
It might not seem obvious, but exercising regularly is important for maintaining gut health. Since exercising reduces overall stress load, it also reduces the negative effects that stress normally has on the digestive system. Take up walking, jogging, dancing, swimming, or even yoga – they’ll all help!
5. Avoid GMOs and Foods High in Pesticides
GMOs and high-pesticide foods are very damaging to our gut microbiome. Glyphosate (aka. Roundup) damages the delicate encasing of the bacteria in our gut, which we depend on to feel good, and properly absorb nutrients from the food we eat.
6. Avoid Antibiotics
While the use of antibiotics in extreme cases is permissible, a lot of the time, doctors prescribe antibiotics when they aren’t really needed. Using antibiotics completely changes your gut microbiome, promoting unfriendly groups of bacteria like firmicutes, which increase your risk of obesity. If you must take antibiotics, make sure you’re also taking probiotics at the same time, and after your round of antibiotics, double up on a high-quality probiotic (like those mentioned above) for at least a year or more.
7. Meditate and Relax
Too much stress doesn’t only affect your brain – but it affects your gut bacteria, too. Take time each day to meditate and relax. Just 15 minutes in the morning or evening is enough to calm the brain.






[…] that even the most advanced scientific breakthroughs are having issues cracking. One of these is depression. And while the conventional approach to depression involves a combination of antidepressant agents […]